Two Fordham researchers are using laser and fiber optic technology to detect nanoscopic particles of the human papillomavirus (HPV).
Stephen Holler, PhD, assistant professor of physics, teamed with Patricio I. Meneses, PhD, associate professor of biological sciences, as well as several undergraduate and graduate students. They are using a technology called prism coupling to detect different genotypes of nanoscopic virus particles.
“Nobody is looking at HPV with this technology,” said Meneses.
Learning from the Whispering Gallery
Just over three years ago, Holler and colleagues from the Polytechnic Institute of New York University and City University of New York made a media splash when they when they used a whispering gallery mode biosensor to detect the smallest known aqueous-borne RNA virus.
At Fordham, Holler set about recreating the whispering gallery lab with some of his students.
But in a trial-and-error learning process, they veered from the conventional whispering gallery designs and opted instead for a prism coupling procedure. Holler said the prism coupling was a more robust process that allowed physics students to construct the apparatus faster and begin research with their biology colleagues. It also will more easily enable the testing of a greater number of viruses simultaneously.
Measuring HPV with Fiber Optics
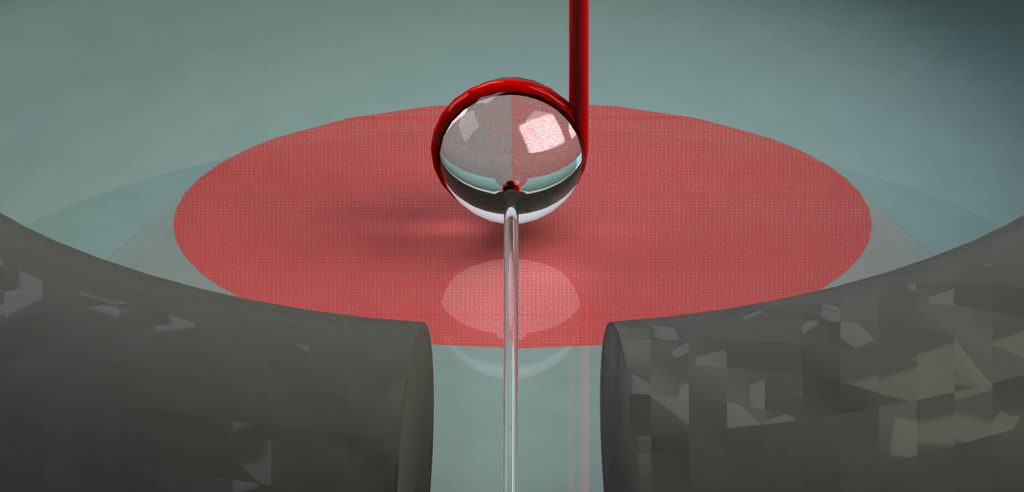
Holler explained that a fiber optic is formed into a very small ball (a miscrosphere) some 100 microns in diameter, and about the same as a strand of hair. The ball sits atop a glass prism that is shot through with laser light. Light circulates within the ball and a specific amount leaks out.
From above, a microscope measures the light leakage. When antibodies are placed onto the surface that affects the leakage, when viruses bind to the antibodies on the surface it effects the leakage and this allows for measurements of a very small number of virus particles.
“The specificity of our work for HPV is not just to measure small particles but also to detect the different types of HPV,” said Meneses.
Meneses said that there are hundreds of types of HPV, but only certain types cause cervical and other human cancers. HPV 16 is the type most commonly associated with oncogenesis.
As different viruses can be recognized by specific antibodies, the sphere can be covered with distinguishing antibodies for HPV 16, HPV 18 or others.
Currently, the HPV vaccine covers HPV 16 and HPV 18. One of the benefits of the new machine being developed in the Rose Hill campus labs is the potential to quickly identify what type of virus are found in individuals, and thus in a population or region.

The light in the whispering gallery mode is represented as the ribbon around the perimeter of the sphere.
Saving Lives
“If this were to work in an ideal world, we could have five or 10 beads on the prism at a time, detecting the various HPV genotypes,” said Meneses. “There are more vaccines coming onto the market that will cover more types of viruses, so there will be a need to identify the HPV types in the target populations.”
While the project is still early in its development, Holler said that ultimately the goal is to make the apparatus portable and capable of being battery-operated.
“The potential is great,” said Holler. “We’ve already demonstrated that bio-detection is possible.
“Here the goal is to create an inexpensive, robust instrument that can be taken out to a rural area for testing where there are no labs, and that potentially could save some lives.”