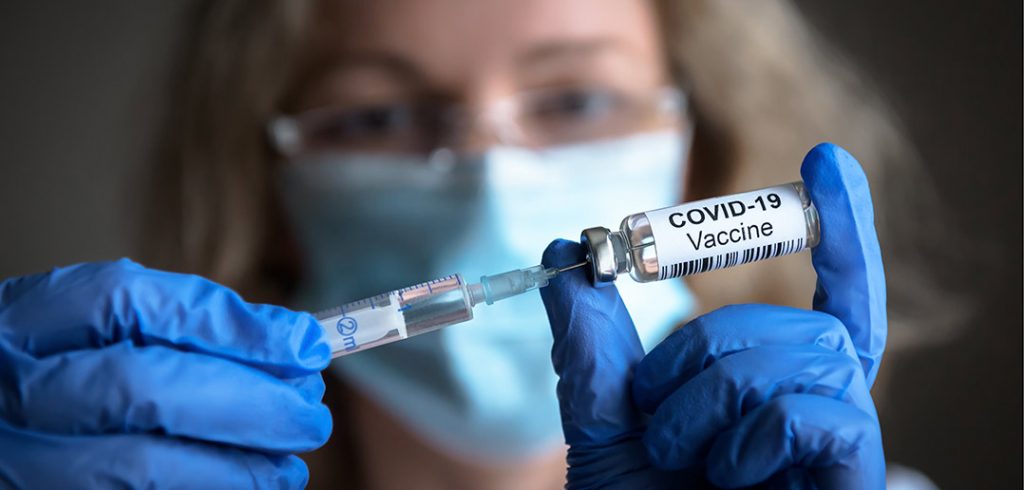
“Vaccines don’t save lives; vaccination saves lives,” said Ronald A. DePinho, M.D., FCRH ’77, a distinguished researcher at the University of Texas MD Anderson Cancer Center, during a virtual panel discussion on Monday, December 21. “It’s very important that when you have the opportunity to get vaccinated, please get vaccinated.”
He and fellow panelist Michael Dowling, GSS ’74, a Fordham trustee and president and CEO of Northwell Health, the largest health system in New York state, emphasized the safety and efficacy of vaccination, as well as the public health messages that need to be widely spread.
“The COVID crisis is not over,” said Dowling, who described a surge of COVID-19 patients in Northwell’s hospitals over the past three weeks. Both he and DePinho said that wearing masks, socially distancing, and washing hands will remain critical well into the new year to prevent the spread of the disease.
The two Fordham graduates were the panelists for “Our COVID-19 Odyssey: Vulnerabilities Revealed, Historic Scientific Progress Achieved, and a Nation Awakened,” hosted by the Fordham University Alumni Association (FUAA) as the inaugural event in its Insights and Impact speaker series. Fordham Provost Dennis C. Jacobs, Ph.D., moderated.
The event came exactly one week after Northwell made history by administering the first doses of the vaccine developed by Pfizer and granted emergency use authorization by the Food and Drug Administration on December 11. A second vaccine, developed by Moderna, got the same approval four days ago, on December 18.
Masking Up
With healthcare workers and other vulnerable groups getting first priority for the vaccines, the general public would probably be receiving the vaccine in the late spring, making continued precautions necessary, Dowling said.
Masks are a good idea even for those who are vaccinated, since it’s still not fully known whether they can transmit coronavirus after getting the shot, DePinho said. “I think it’s going to be very hard” for this to happen, he said, “but until we really know, the safe and proper thing to do, the compassionate thing to do to protect others, is to wear a mask.”
Dowling said he thinks masks are here to stay, not only because of uncertainty about how long the coronavirus vaccination lasts but also because of their potential for suppressing the seasonal flu.
An Astounding Advance
The Pfizer and Moderna vaccines were each found to be 95% effective in clinical trials, a rate that DePinho called “astounding,” noting that the FDA standard was just 50%.

“This is an extremely safe vaccine and a very effective one,” said DePinho, professor, past president, and Harry Graves Burkhart III Distinguished University Chair in the Department of Cancer Biology at MD Anderson.
“You’re more likely to get harmed driving on the way to the hospital to get the vaccine than you will actually getting the vaccine,” he said.
They both emphasized that aftereffects like a sore arm, fatigue, or low-grade fever are actually a good thing. “It means the vaccine is working,” Dowling said.
He and DePinho addressed safety concerns such as allergic reactions that might be brought on by ingredients within the vaccines. The medical profession is “very skilled at handling those allergic reactions,” DePinho said. “On the other hand, as Michael will attest to, you do not want to get this virus.”
“This is a virus that kills,” and brings long-term problems like diminished lung capacity, strokes, and cardiac problems, he said. “This is a bad virus with enormous capabilities.” Compared with the manageable side effects of vaccines, he said, “the decision should be quite clear.”
At Northwell, people have to stay for 15 to 20 minutes after being vaccinated, and staff members are there to address any negative reactions, Dowling said. Most recipients feel few side effects, he said.
Making the Case
Overcoming skepticism—which exists even among healthcare workers—and convincing enough people to get vaccinated to achieve the estimated “herd immunity” threshold of of 70% will be “one of our biggest challenges,” Dowling said.
The stakes are high, DePinho said. “We’ve got to vaccinate about 5.6 billion people for herd immunity across the globe. Until we do that, this virus is going to keep coming back in waves, and as we just learned in the U.K., this virus mutates, it adjusts, it becomes more virulent, more infective.”
“So we have to really get ahead of this quickly and decisively, and it’s going to require worldwide immunization. No one’s safe until we do that.”
Dowling described the challenges of administering the vaccine, noting that the one from Pfizer has to be stored at minus 70 degrees Celsius and requires two doses 21 days apart.
DePinho said global vaccination efforts could be helped along by rapid scientific advances of recent years, like new messenger RNA-based therapeutics or nanotechnology that could be used to create dry powder vaccines that can be stored at room temperature. “Globally, those kinds of technologies are going to have a huge impact,” he said. “We’ve seen science really transform our ability to go from essentially a cold start to vaccinating people and protecting the public.”
Jacobs invited a comment about vaccines from Sally Benner, the vice chair of the FUAA advisory board who kicked off the event by introducing the panelists. Benner is the associate vice president of development for medical sciences at the University of Oxford, which developed a coronavirus vaccine that was licensed by AstraZeneca and is awaiting a trial in the U.S.
The speed of the vaccine’s development came from scientists having “a very long runway,” she said—they began working on a “Disease X” similar to the coronavirus five years ago at the urging of the World Health Organization, she said.
Community Leadership
In addition to vaccines, ending the pandemic requires a “strong, sophisticated communication mechanism and campaign to get people to understand [getting vaccinated] is the right thing to do … if you want to protect your community and yourself,” Dowling said.
He’s involved in statewide discussions about how to overcome people’s reluctance, particularly in African American and other minority communities that are disproportionately affected by the virus.
Clergy, pastors, and other leaders in those communities can play a valuable role by getting vaccinated, talking to others about it, and advising on how best to communicate the need to get vaccinated, he said.
Sandra Lindsay—the intensive care nurse who was the first Northwell employee vaccinated—is Jamaican, and has been “very vocal” in her community about the safety of the vaccine, Dowling said.
Celebrities could also play a role, he said, noting how Elvis Presley publicly took a vaccine for polio in 1956 to encourage young people to take it.
DePinho said the Catholic Church is “an incredible” platform for encouraging vaccination, since Pope Francis understands the importance of disease prevention and vaccination. Fordham and WFUV, the University’s public media station, could also spread the message, he said.
Education and Preparation
“Knowledge is disease’s greatest vulnerability,” DePinho said. “Vaccines have been one of the great triumphs of the last century,” he said, going through a list of maladies that people simply don’t think about anymore.
“We have to try to stay ahead of these viruses. We’re under constant assault,” he said. “This won’t be the last pandemic.”
“In much the same way we have ‘war games,’ we need to have ‘germ games’” to foster preparedness, he said.
Last spring, New York Governor Andrew M. Cuomo, FCRH ’79, named Dowling co-leader of a statewide council on expanding hospital capacity in the face of the pandemic.
Asked about lessons learned, Dowling said hospitals learned “to cooperate an awful lot more together” and constantly share information, with stronger hospitals backing up the weaker ones. Northwell has also formed reciprocal agreements with other large health systems around the country to share staff as needed when crises arise. He said he hopes for broad strategies to be developed in the U.S. and globally to prepare for future pandemics.
A Sputnik Moment
DePinho said the pandemic is “like our Sputnik moment,” referring to the 1957 satellite launch by the Soviet Union that spurred new technological, educational, and other advances in the United States. The pandemic has brought tragedies but also opportunities to improve health care delivery, infrastructure, “and the disparities that exist in our society.”
“We need to invest in health care and prevention, not just disease care, particularly for underserved communities,” he said. “In much the same way that we had our Sputnik moment, hopefully in the decades ahead we will look back on ‘the COVID moment’ where we transformed the way that we work together to serve the public good.”
In closing remarks, Joseph M. McShane, S.J., president of Fordham, said the event delivered a clear message: “We should be advocates for, ambassadors for, evangelists for the vaccination programs,” he said. “Tell people in all the worlds that you inhabit that this is the way toward a brighter future.”
He noted the date, December 21, the winter solstice and the shortest day of the year. “Light will grow from this moment on,” he said, “and part of the light [that]will grow is the light that we derive from listening to you, sitting at your feet, and hearing all the experience-based wisdom that you had to offer.”
The Fordham University Alumni Association (FUAA) launched the Insights and Impact speaker series to showcase Fordham alumni making a positive difference in society. On January 21, the FUAA will host its annual Recognition Reception. Visit the event page to learn more and register.